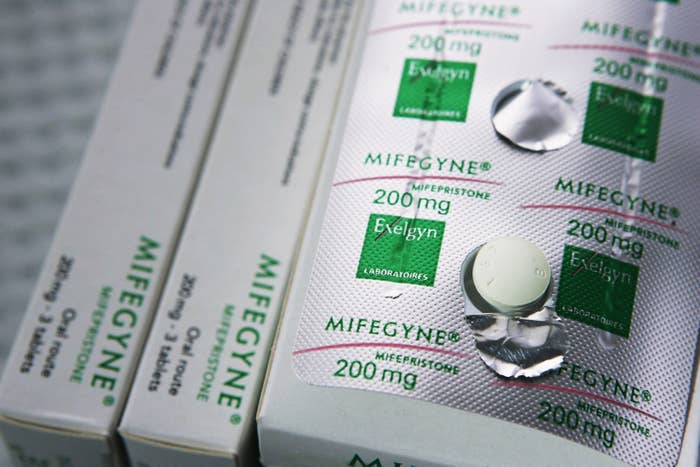
Many women in Britain who turn to the internet to get hold of abortion pills do so because they are unable to access the procedure via a clinic, according to new research.
Data published today in the journal Contraception gives fresh insight into the reasons behind a dramatic recent increase in women in Britain seeking to illegally carry out early medical abortions at home, despite the procedure – which doesn't require surgery – being legally available in clinical settings in England, Scotland, and Wales.
Campaigners believe the findings strengthen the case for the now 50-year-old Abortion Act 1967 to be reformed and updated in line with medical advances.
Long waiting times, distances to a clinic, work and childcare commitments, and lack of eligibility for NHS services were among the most common reasons for seeking abortion pills online given by women who contacted Women on Web, a nonprofit organisation that sends the pills to those in countries where the procedure is illegal.
Researchers from the University of Texas found that more than 500 women from Britain contacted Women on Web between November 2016 and August 2017.
Among the reasons women gave for approaching Women on Web, 49% were due to obstacles they faced accessing the drugs Mifepristone and Misoprostol in a setting where they could be legally administered.
Medical abortion is suitable for terminating pregnancies of up to 10 weeks gestation. Seventy-seven percent of the women who contacted Women on Web during that time period were less than 7 weeks pregnant, and 23% were between 7 and 10 weeks pregnant.
"Unfortunately, my local area is somewhat out of the way. I do not drive and cannot afford the public transport to attend the 3-4 appointments that they require to complete the abortion," Lisa*, a 25-year-old from England, told researchers.
She added: "I'm really desperate and I've been told there is a 3-week wait, I'm really distressed and I just want the procedure over and done with."
Campaigners believe the findings underline the need for a revision of the Abortion Act, which means early medical abortion can only be administered in a licensed clinical setting despite mounting evidence, supported by the World Health Organisation, that the drug is safe to take at home.
"It’s another reflection of how out-of-date that piece of legislation is," Clare Murphy, director of external affairs for the British Pregnancy Advisory Service (BPAS), told BuzzFeed News.
Thirty percent of the women surveyed said they had been faced with waiting times for a medical abortion at a clinic that would take them over the 10-week limit for an early medical abortion, meaning they would instead need to undergo a more invasive surgical procedure in order to end the pregnancy.
“I am currently between 7-8 weeks pregnant and want a medical termination however all abortion services in the UK are heavily backed up and cannot offer me 170 appointment for over three weeks," Alison*, a 30-year-old woman in England, told researchers.
"I've called every service provider in my area and also gone through my GP," Alison, who wished to carry out the procedure at home using pills obtained online, continued. "I can’t endure the mental anxiety of staying pregnant for another three weeks and then having a surgical procedure."
Almost 20% of women surveyed said they contacted Women on Web because they weren't able to attend the multiple appointments for a medical abortion that are required by law. The procedure involves Mifepristone being taken to induce a miscarriage, followed 24-48 hours later by a dose of Misoprostal to expel the miscarriage. Under UK law, both drugs must be taken at a licensed clinic when used for abortion procedures, meaning women cannot be sent home with the second drug – so two appointments, days apart, are necessary.
Among the most common reasons women cited for not being able to attend two appointments that were days apart were living a long distance from a clinic, being unable to take multiple days off work, and not having sufficient childcare provisions.
"I am only two weeks pregnant, I already have three kids and I am a single working mum," said Linda*, a 31-year-old from Scotland.
"I am unable to go to the hospital as I do not have the funds to pay for childcare while I would be in there. I am unable to take time off work and I can't tell my family so there is no one I can ask to look after the kids. I really need to do this in my own home.”
Thirty percent of women surveyed said they wanted to carry out an abortion in their own home because of concerns around privacy, particularly those who lived in areas with close-knit communities who feared they might be seen attending an abortion clinic.
Additionally, 18% said violent or controlling circumstances made it difficult for them to obtain the procedure in a clinical setting, with just over 11% of those women fearing the threat of violence.
"I'm in a controlling relationship, he watches my every move, I'm so scared he will find out, I believe he's trying to trap me and will hurt me," Susan*, 30, from England, told researchers. "I can't breathe. If he finds out, he wouldn't let me go ahead, then I will be trapped forever. I cannot live my life like this.”
Murphy of BPAS told BuzzFeed News she was "taken aback" by the number of women who appeared to face barriers in accessing the procedure via a clinic. "I don’t think any of us had any idea that these were the kind of numbers we were looking at," she said.

While BPAS does offer the option of simultaneous administration of the two drugs at a clinic, making only one appointment necessary, Murphy stressed that this is by no means an ideal solution, as it reduces the effectiveness of the procedure and can increase the severity of unpleasant side effects such as nausea.
She said the research indicated that it should be easier for medical abortion drugs to be administered outside of a registered clinical setting, and that perhaps GPs could even directly prescribe the drug.
Earlier this year a parliamentary bill was put forward by Labour MP Diana Johnson to reconsider current abortion law in the UK to allow women to be able to legally access abortion more easily.
Murphy said: "This research really pinpoints some of the issues with how the law shapes provision, and I think the way in which medical abortion has to be delivered in this country is absolutely a case in point." When the current abortion law was written 50 years ago, she said, it could not have been anticipated the availability of drugs that allow the safe termination of pregnancy outside of a clinical setting.
Research published by the British Medical Journal in April showed that 94% of women who took part in a study exploring the safety of taking abortion pills with no medical supervision reported no adverse effects.
Dr Abigail Aiken, who wrote both the BMJ paper and the new study on barriers to abortion services, told us she hoped that the research would help make medical abortion more accessible for marginalised women.
"I think [marginalised women] are the ones who are perhaps not being talked about so much by the people who are putting policies together," she said.
“To close the healthcare gap for the most vulnerable and marginalised, we need to find innovative ways to bring services to people where they are."
Aiken said she believed policy change was necessary to allow new models of delivery of early medical abortion that would make it more accessible.
The National Institute for Health and Care Excellence (NICE) is in the early stages of revising its guidelines on abortion care, which could help to shape policy, and its areas of current concern mirror those highlighted in Aiken's research.
A NICE spokesperson said recent developments in abortion services, including the refinement of early medical abortion procedures, could significantly reduce costs to the NHS, but agreed that variations in local services could be restrict access to the procedure.
"Accessing termination of pregnancy services may be difficult for women who live in remote areas; who are in the second trimester of pregnancy; or who have complex pre-existing medical conditions or difficult social circumstances," the spokesperson said.
"[New guidelines] will help ensure that termination procedures are carried out based on the best available evidence, and that services provide safe and appropriate access to women who require a termination of pregnancy."

Labour MP for Walthamstow Stella Creasy, who recently was instrumental in securing free NHS abortion services in England for women travelling from Northern Ireland, agreed that access to early medical abortion should be improved.
"The earlier an abortion takes place, the less invasive for the woman concerned, so access to treatment is vital as well as more cost-effective for the NHS," Creasy told BuzzFeed News.
"This research suggests women could be left waiting too long to see a doctor because of shortages of GP appointments and that some are then turning to the web for help. The Department of Health must urgently review how services operate to ensure no woman is forced to have an operation because she can't get a simple appointment."
A DoH spokesperson told BuzzFeed News there were no current plans to revise abortion services in England. “All women who require abortion services should have access to high quality and safe care," they said.
"It is a widely available procedure that is safe and regulated, with around 180,000 women accessing abortions a year. All abortion providers must have protocols in place for helping vulnerable groups.
"In addition to information on NHS Choices, there are also helplines set up to provide advice."
