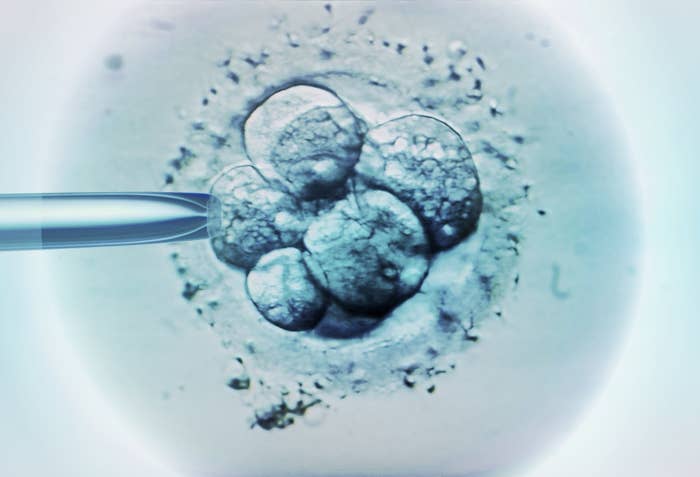
The first "three-person" pregnancies could go ahead as soon as next year, after the Human Fertilisation and Embryology Authority (HFEA) approved the use of mitochondrial donation to allow women with mitochondrial disease to have healthy children. The decision follows the recommendation of a panel of experts put together by the HFEA who said the technique should be cautiously put into practice.
Scientists have welcomed the decision. Professor Sir Mark Walport, the government's chief scientific adviser, said in a statement: "The UK leads the world in the development of new medical technologies. This decision demonstrates that, thanks to organisations like the HFEA, we also lead the world in our ability to have a rigorous public debate around their adoption.”
Most of the cells in our body contain many thousands of mitochondria, organelles that provide the cell with energy. They are descended from bacteria and have their own DNA, unrelated to the DNA in the rest of our cells. You inherit your mitochondria from your mother, and when mitochondrial DNA mutates it can cause severe diseases.
However, it is possible, using new in-vitro fertilisation (IVF) techniques, to take the nucleus out of an egg and implant it into a new one, leaving almost all of the mutant mitochondria behind and – it is hoped – preventing mitochondrial disease from being passed to children. Last year, parliament voted to make the techniques legal, and the HFEA has since been looking at whether and how to make it available.
A spokesperson for the HFEA told a press briefing following the panel's recommendation that, if everything goes smoothly, the first attempts to produce a baby using the techniques could go ahead early next year.
Mitochondrial disease is rare – affecting about 1 person in 10,000, and perhaps around 3,500 women in the UK, according to the HFEA panel. But the condition is "cruel", Liz Curtis, founder of the Lily Foundation, told BuzzFeed News. Her daughter Lily had mitochondrial disease and died at 8 months old. "It's a very, very cruel disease," she said. "It can be fatal, and if it doesn't take the child very young in life, over time it strips their body of energy, slowly attacking each organ until they fail.
"Watching your child die, knowing there's no cure and nothing you can do, it's cruel, and knowing you carry the gene that will more than likely be passed on to other future children, it's a double blow." She said the HFEA recommendation is a "huge step forward".
The current recommendation for women who have a family history of mitochondrial disease and want to have a baby is "pre-implantation genetic diagnosis" (PGD). Women undergo normal IVF treatment – their eggs are harvested, along with their partner's or donor's sperm, and they are fertilised in the lab. Before implantation, the levels of mutant mitochondria in the fertilised embryos are tested. If they are low enough, they are implanted, and often produce children with few or no symptoms.
PGD is an "excellent" option for women who only have low levels of mutant mitochondria, Frances Flinter, a professor of clinical genetics at Guy's and St Thomas' NHS Trust, told a press briefing. However, for women who have very high levels of mutant mitochondria, PGD cannot offer any help, because it will be impossible to make safe embryos using their eggs.
Also, she said, if you set the "safe" threshold too low, you may not get any viable embryos, whereas if you set it too high, the disease may manifest itself in the child. "PGD is very much a risk-reduction technique," she said. "It doesn't eliminate the disease but it reduces the likelihood of severe symptoms."
Mitochondrial donation techniques – of which there are two main kinds, "maternal spindle transfer" (MST) and "pronuclear transfer" (PNT) – reduce the risk further, Robin Lovell-Badge, a professor of developmental genetics at the Crick Institute and another member of the HFEA panel, told the briefing. "If you're looking at a new technique, you want it to be better than the old technique," he said.
Both MST and PNT reduce the levels of mutated mitochondria in embryos to less than 2% and sometimes less than 1%, he said, compared with "safe" thresholds for PND that are sometimes as high as 30%. Sometimes, after donation, an apparently healthy embryo can "revert" – the low levels of mutant mitochondria can go back up to a dangerous level. In studies, including one published recently in Nature, that seems to happen about one time in every six or eight.
But Flinters told BuzzFeed News that it would be very unlikely that this would lead to a child being born with mitochondrial disease, because it would be detected through testing during the pregnancy. "We recommend that parents are offered prenatal diagnosis at around the 15th week of pregnancy," she said. "From 15 weeks to birth the levels of healthy mitochondria are very stable."
As far as would-be parents are concerned, the mitochondrial donation procedure would be indistinguishable from normal IVF, Darren Griffin, a professor of genetics at Kent University, told BuzzFeed News. "The patient wouldn't know any different," he said. "There's a donor involved, but other than that it's the same."
A would-be mother would be given medication to suppress her menstrual cycle and boost her egg supply. Then eggs would be harvested through the vagina, using an ultrasound to guide the procedure. In MST, the nucleus of the egg would be taken out at this point and implanted in a healthy egg from which the nucleus has been removed.
Then the egg would be fertilised with sperm. In PNT, the fertilised nucleus of the new embryo would be removed at this point and implanted into a healthy embryo.
Then the embryos would be tested for levels of mutant mitochondria, and those with sufficiently low levels would be offered for implantation into the woman's womb, using a catheter, as in normal IVF. The patient would be offered amniocentesis, a test to see if the foetus is still healthy, at around 15 weeks.
Licences to carry out the technique will be granted by the HFEA to centres that apply, and then permission will have to be given on a patient-by-patient basis. "I can't see it being huge numbers of people using it," said Griffin. "Perhaps hundreds a year, no more than that.
"But the diseases it causes are so horrendous, and the means of treating it are so limited."

