Although the Zika virus is best known for damaging the brain of a developing fetus, it may also trigger long-term harm in the memory centers of infected adults.
That’s according to a provocative study of adult mice published today. Researchers saw the virus kill stem cells in the animals’ brains that were responsible for healing and forming new memories.
But other experts say the results are far too preliminary to have implications for addressing the human Zika epidemic, which has just hit Florida in earnest.
Scientific journals appear to be in a hurry to publish Zika-related research, Avindra Nath, clinical director of the National Institute of Neurological Disorders and Stroke, told BuzzFeed News, adding that he was disappointed the new study only used mice with particularly weak immune systems and didn’t follow the animals for longer than a few days.
“To extrapolate to humans would be a mistake at this time,” Nath said. “You already have a whole lot of paranoia in the public as it is. To add this on top of that, with data that is preliminary, is a disservice.”
Although Zika has been linked to rare cases of a neurological condition called Guillain-Barré, most healthy adults who contract the virus show only mild signs of infection, such as a fever and rash. That’s one of the reasons Nath is skeptical of the findings.
The scientists who carried out the new study agree their findings should not change the way public health authorities are monitoring people with Zika. But that doesn’t mean that the study isn’t relevant to people, they say. In adults who have been infected with Zika, there may be long-term neurological effects that have not yet come to light.
“Perhaps Zika is not innocuous in adults,” Joseph Gleeson, a professor at Rockefeller University who led the study, told BuzzFeed News.
Gleeson said he is not suggesting that every patient exposed to Zika be screened for neurological symptoms. “But I am suggesting we keep an eye out for patients who show evidence of brain infection following Zika and follow them over time and see if they have effects on cognition,” he said.
From infecting chunks of brain-like tissue in a petri dish with the virus, researchers already knew that Zika has an affinity for “neural progenitor cells” — shape-shifting stem cells that are able to transform to fill various roles in the brain.
These results led to the theory that when pregnant women contract Zika, the virus hones in on the developing brain of the fetus, which is rich with neural stem cells, and obstructs normal growth, resulting in the shrunken heads of infants that are the hallmark of the infection.
The new study, published in journal Cell Stem Cell, shows for the first time that Zika can also attack these stem cells in the brains of an adult mammal.
“Does it really surprise me that this is going on? No. But I am glad to see it,” Shannan Rossi, assistant professor of pathology at the University of Texas Medical Branch, told BuzzFeed News. “I think it’s really important to show that what we manipulate in a petri dish is also [true] in a mouse.”
Mice are able to fend off the Zika virus without getting sick, so Gleeson’s team worked with a laboratory strain that were genetically modified to weaken the immune system.
They injected the virus into the bloodstream of mice that were 6 weeks old — which corresponds to an age of about 20 years in people — and after six days, killed them and sectioned their brains.
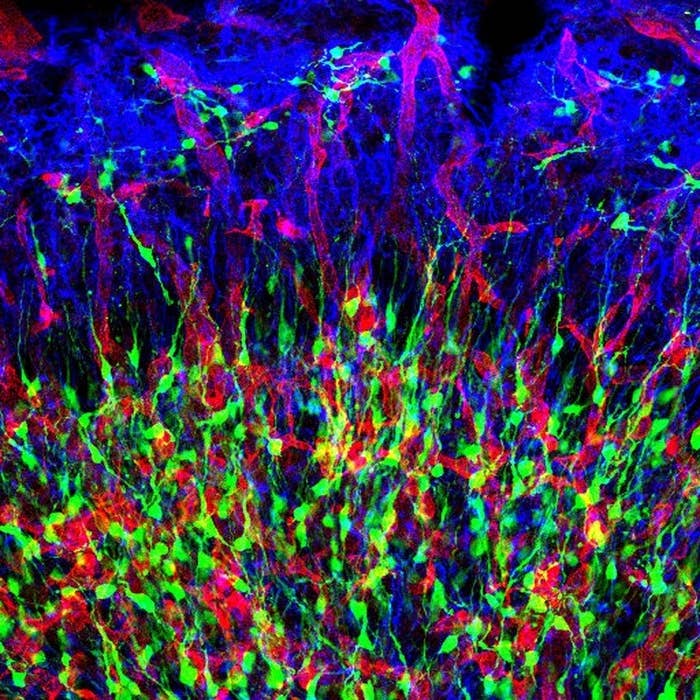
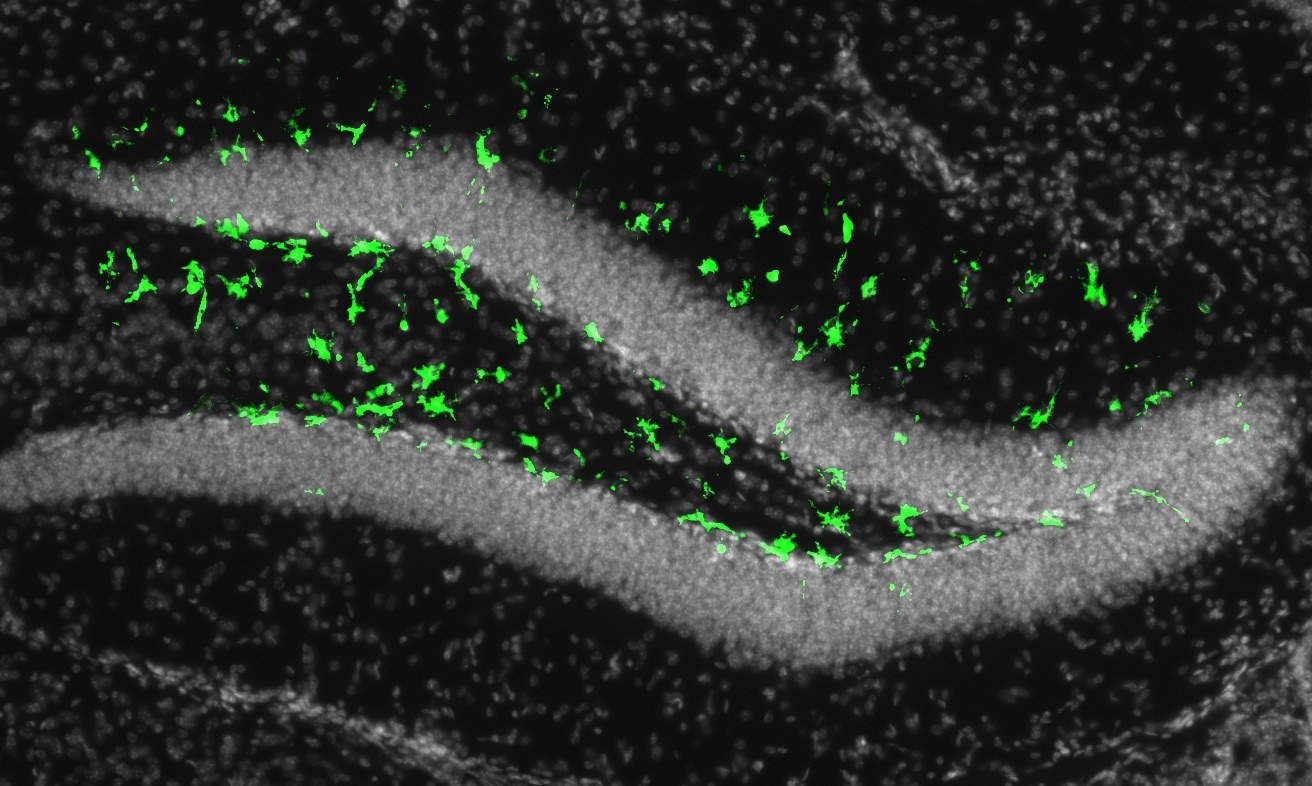
“We found that most of the brain had no vulnerability to Zika,” Gleeson said. “It was only in these stem cell populations — they lit up like a Christmas tree, they were very bright.”
Though studies like these in mice are important stepping stones to discoveries about the virus’s impact on people, there are also reasons the virus could behave quite differently in healthy adults.
For one, the extremely weak immune system of these mice could allow the virus to behave differently compared to being fought off by a healthy person. “Your average human walking down the street is going to be able to mount that response just fine,” Rossi said.
Gleeson plans to next investigate mice that have a stronger immune systems and can survive a bout with the virus. Those would be observed over the course of their lifetime and tested for cognitive changes following the infection.
Those are the results Nath at the federal government would like to see before making any changes to how public health officials monitor people with the virus.
In particular, the results should not shift the focus of the public response away from pregnant women, who are most seriously harmed, Rossi said. If rarer brain infections in adults do indeed happen, they can wait. “I don’t think at this time that it’s the right place to be putting our efforts,” she said.
She acknowledged that rare infections and long-term effects in adults will become important — but only after the heat of the epidemic has passed, months or years from now.
