
When Nicole Cronin’s parents sent their daughter from suburban New Jersey off to a Florida rehab to treat her opiate addiction, they hoped it would help free her from the relapses they’d watched her cycle through at home.
Instead, she ended up dead at 20 years old. Her body was found in a cheap motel a few miles from the $800-a-month halfway house her parents were footing the bill for, according to a lawsuit filed by her family.
Nicole died in Delray Beach, the “recovery capital of America.” The oceanfront vacation spot is home to thousands seeking sobriety — as well as scam artists who prey on addicts and their insurance plans.
The U.S. is in the middle of an oxycodone and heroin epidemic. The rise of prescriptions for opiate painkillers, and the “pill mills” that kept the scripts flowing, built a steady and captive user base. Once pill-mill crackdowns and other drug war initiatives cut off that supply, heroin dealers were quick to snatch up market share.
When addicts want to get clean, the most common path, at least for those who can afford it, is a brief chemical detox followed by a 28-day inpatient rehab. In South Florida, rehab is often followed by a much longer stint living in a halfway house (typically a low-rent apartment) with other recovering addicts. People staying in those “sober living” homes are often encouraged to get additional support from outpatient programs that offer one-on-one counseling, group therapy, and 12-step programs.
But there’s little scientific evidence that any of these recovery approaches work.
Most inpatient rehab programs last for 28 days only because of a historical oddity: It’s the standard cap insurance companies agreed to decades ago, when rehabs first became a regular part of addiction treatment. And many intensive outpatient models require abstinence from all opiates, even though it runs counter to scientific research showing that certain opiate medications, such as methadone, buprenorphine, and suboxone, slash the death toll of addiction.
Nobody systematically tracks the success rates of recovery programs. But addiction experts contacted by BuzzFeed News agree that, no matter what kind of recovery, the relapse rate for opiate addiction is dismal — perhaps as high as 90%.
That means that even in recovery facilities run by educated people with good intentions, addicts bounce in and out, and are often undone by easy access to street drugs.
Sometimes it’s even worse. Stories abound in Delray Beach of halfway house owners charging insurance companies thousands of dollars a month for simple urine tests, collecting illegal referral fees from rehab programs, and even finding ways to get addicts drugs in hopes that they will relapse.
The feds are beginning to take notice. At the end of 2014, FBI and IRS agents raided a handful of facilities in South Florida, including Halfway There, where Nicole was staying when she died, and its sister organization, an outpatient program called Real Life Recovery, which was licensed by the Florida Department of Children and Family Services to provide counseling to addicts.
Nicole’s family is suing Halfway There for wrongful death, alleging that the halfway house’s staff took her to the motel because she was high, without ever seeking medical care.
Both Halfway There and Real Life Recovery went out of business earlier this year, according to Judd Brazer, the general manager of the company that purchased Real Life Recovery’s assets. Eric Snyder, who owned Halfway There and Real Life Recovery, declined to answer detailed questions that BuzzFeed News sent through Halfway There’s lawyer, Bryan Yarnell.
“The passing of Nicole Cronin was tragic,” Yarnell responded by email, adding that he cannot address specific facts of the case because of pending litigation. “However, my client is confident that when all of the facts are brought forward, that the wrongful death action which has been filed against it will be found to have no merit.”
There are no doubt many addicts who find help in Delray Beach (as some of the Facebook reviews of Halfway There attest). But there’s no denying that the city’s recovery industry is full of bad actors.
“We have some of the best of the best, and some of the worst of the worst, in Delray Beach,” Paul Cassidy, the chief operating officer of Access Recovery Solutions, a treatment center in Delray Beach, told BuzzFeed News. “Anywhere there’s money to be made you’re going to get people who don’t have the right intentions.”

Nicole Cronin was in high school when she first got into drugs. She started with pot, then, after she met the dealer boyfriend her parents refer to only as “The Scumbag,” she got into opiates — first painkillers, then heroin.
Her parents found out about their daughter’s habit when her mother, Myra Cronin, was called out of work to come pick up her kid at school. Nicole had seemed high, her mom recalls, so the school searched her purse, found drugs, and called the police. Because it was a few days before her 18th birthday, Nicole was dealt with as a juvenile.
Nicole’s family immediately put her into an outpatient program down the street from their New Jersey home. Eventually the program’s staff suggested she go to a 28-day facility for more intensive care. She started college twice, both times getting kicked out within weeks for using drugs.
Her relapses took her back and forth between inpatient treatments and intensive outpatient programs, until finally her clinicians recommended that Nicole go to Florida, far from her dealers and addict friends.
The day before Christmas in 2011, when she was 19, Nicole got on a plane bound for a South Florida rehab. She never came home.
In Florida, she fell into a trap familiar to many addicts: a constant cycle between chemical detox, 28-day programs, halfway houses, and relapses.
Myra paid for her daughter’s rent at Halfway There. It was an abstinence-only program that required residents to attend daily 12-step meetings — no methadone or suboxone allowed. As a 2013 post on Halfway There’s (now defunct) blog put it: “Suboxone allows people to avoid experiencing the full effects of withdrawal so they don’t ever adjust their bodies and their brains to a drug free life. If a person never truly has to get off of a drug to be considered ‘clean’ or normal then why would they?”
Nicole stayed at Halfway There for four days. On the night she died, she spoke by phone to a friend she knew from an earlier stint in a different rehab, the friend told BuzzFeed News. (Because of the stigma of addiction, he agreed to talk only on condition of anonymity.) According to this friend, Nicole was looking forward to starting a new job at Panera Bread the next day.
But later that night, the staff of Halfway There found her high on opiates, according to the lawsuit filed last year by Nicole’s parents. Halfway There, like most sober homes, kicked out anyone who relapsed, according to a person who worked at Halfway There in 2013 and spoke to BuzzFeed News on condition of anonymity.
Myra said that she did not receive a phone call from the Halfway There staff that night or anytime after, and that the staff paid for the motel room and left her daughter there alone. (Halfway There declined to answer any questions from BuzzFeed News about what happened that night.)
“It was incredibly negligent not to take her to a hospital or call the police,” Myra told BuzzFeed News, an accusation also made in her family’s lawsuit. “That gross misjudgment led to her death.”
Nicole overdosed on a fatal combination of drugs, including painkillers. Hotel staff found her the next day, “unconscious and unresponsive,” according to the lawsuit.
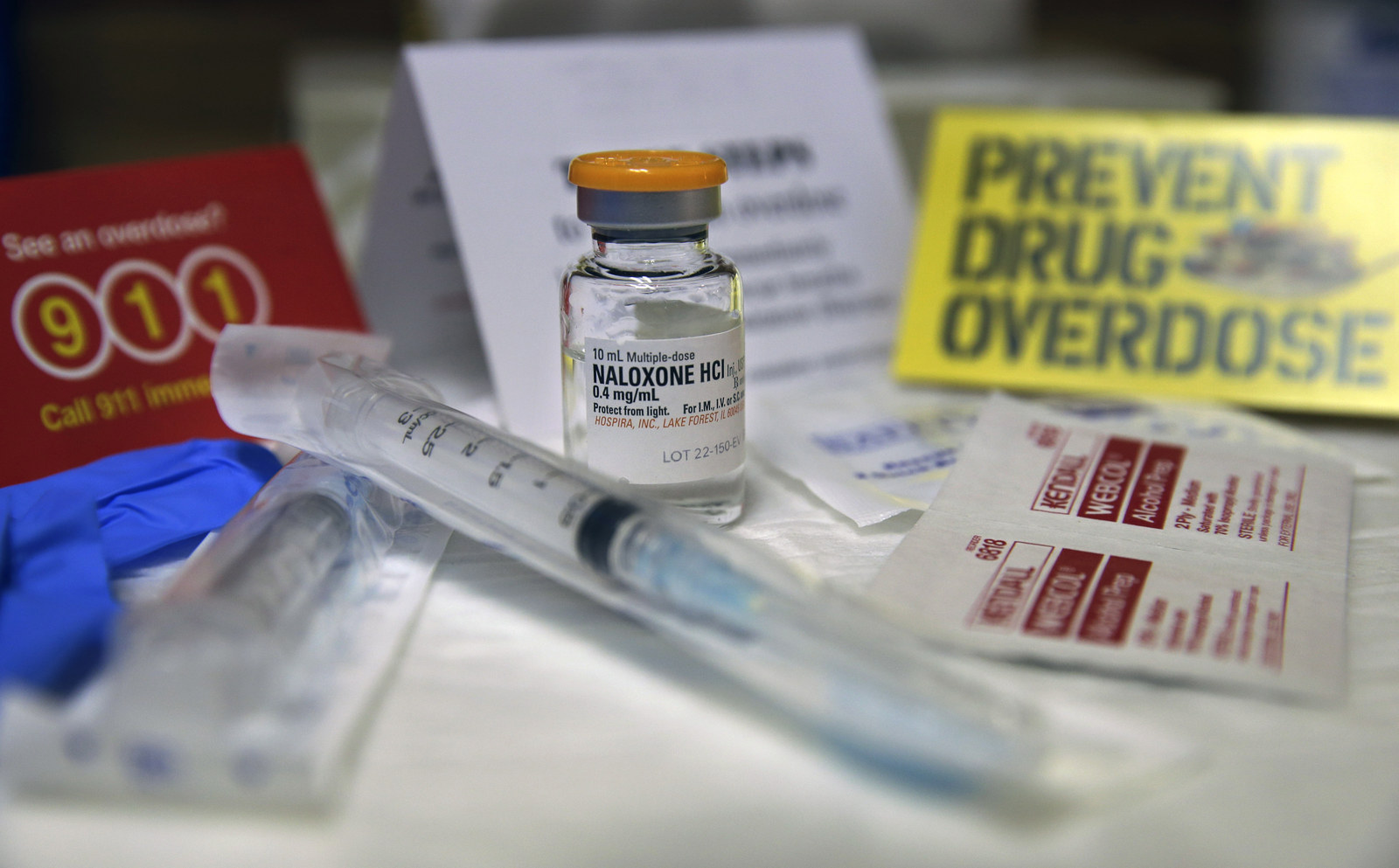
After opiate addicts have come completely off drugs, their tolerance is sharply lowered. If they relapse with the same dose they were used to before — or if they take “enhanced” heroin, which is more concentrated or cut with fentanyl, a more potent opiate — the drugs dampen their body’s urge to breathe. If they don’t get naloxone, an overdose prevention drug, they can die within minutes.
Myra said she first learned about what happened when local New Jersey cops knocked on her door to tell her that Nicole had died in a cheap motel known as a haunt for drug dealers.
Halfway There should never have taken Nicole as a resident in the first place, because she had relapsed so many times already, Susan Ramsey, the Cronin family’s lawyer, told BuzzFeed News. Ramsey specializes in Florida addiction issues and is on the board of Gratitude House, a nonprofit long-term residential program for women in poverty with addiction problems.
“Most people who are chronic relapsers need something other than traditional substance abuse centers,” Ramsey told BuzzFeed News. “They need long-term treatment, where all their psychiatric issues will be looked at. This is not what happens here in South Florida.”
Addiction treatment is big business in South Florida, especially in Delray Beach and the rest of Palm Beach County. Websites boast about 90% success rates and beautiful beach views, as if they’re selling a resort instead of a rehab.
“Florida is a perfect place to seek recovery,” reads the website for Origins of Hope, a treatment facility in Delray Beach. “With a beautiful year round climate, and vacation type atmosphere, it creates an ideal place to come and relax in the natural environment.”
American culture glorifies 28-day programs: Movies like 28 Days and TV shows like Intervention suggest that a sandy beach and a break from the familiar will whisk addicts away from their dangerous habits. In 2007, the New York Times published a glowing piece on Delray Beach, calling it an “oasis” and “the recovery capital of America.”
According to Cassidy of the Access Recovery Solutions treatment center, the recovery industry has really taken hold over the last 15 or 20 years, as more people discover what moneymakers rehabs and halfway houses can be.
Most of them are based on the “Florida model,” which involves addicts attending an intensive outpatient program while working a part-time job and living in a halfway house. This integration, when done right, is said to provide a slow return to the pace and stresses of everyday life.
But when it fails, the consequences can be deadly.
Because relapse is common in early recovery, so are overdoses. Between March and August of this year, 60 people overdosed in Delray. In 2013, at least 590 people died of opiate overdoses in Palm Beach County.
Under Obamacare, insurance companies are required to pay for substance abuse programs. For unscrupulous treatment providers, that means addicts can be a cash cow, racking up bills in the hundreds of thousands of dollars for rehabs and halfway houses that don’t work.
There are no precise estimates of how many people travel from other states to get addiction treatment in Florida, because of the lack of regulation and because medical records are strictly confidential under the Health Insurance Portability and Accountability Act (HIPAA).
But the numbers are huge, according to John Lehman, president of the Florida Association of Recovery Residences, which has been working for more than a year with state and federal officials investigating treatment facilities and halfway houses.
Delray Beach alone has somewhere between 100 and 500 halfway houses, Lehman said, and he estimates that there are up to 3,000 in the state — not to mention the many detoxes, 28-day rehabs, and people who live in non-sober housing while attending intensive outpatient programs.
When those people get out of treatment, they often stick around in the places they’ve become familiar with, go to the NA or AA meetings they know, and keep their local jobs. This settling is reinforced by the 12th step of Narcotics Anonymous, which tasks addicts with bringing the NA message to others who need help.
An easy way to disseminate the message is to take a job at a treatment center, which won’t discriminate against addicts for criminal records, track marks, or other indicators of addiction. And once they’re part of the system, it’s a small leap to opening their own facilities.

In Florida, anybody, even people without any training in medicine or counseling, can rent rooms to recovering addicts on the condition that they not use any drugs.
Ideally, these halfway houses give addicts the social support that’s so important to getting and staying clean. The shared living situation allows them to go to meetings together and help one another navigate the world without drugs or alcohol.
In the early days, according to Lehman, halfway house operators would charge relatively low rents and absorb the cost of occasional drug tests — generally $4 for a plastic cup with test strips to indicate the presence of various substances.
But starting about five years ago, he added, some sober home operators realized they could get a special waiver from the federal government that would allow them to do simple urine analyses — and charge residents’ insurance for them. These waivers don’t require any financial disclosures or background checks.
Some homes began charging insurance companies a few hundred dollars for each urine test.
Some homes began charging insurance companies a few hundred dollars for each urine test, and required residents to do two, three, or even four tests a week, according to Nancy Steiner, the executive director of a halfway house called The Sanctuary in Delray Beach.
Even that wasn’t enough for many outpatient providers and halfway house owners. According to Lehman, many sober homes have made deals with laboratories that can run more expensive chemical tests on the urine, which runs the bill for insurance up into the thousands of dollars. (Florida isn’t the only home to this scam — it’s also been investigated in drug treatment programs in Massachusetts and Kentucky.)
Sometimes the halfway house operators even own the labs. According to an investigation by the Palm Beach Post, 31 local labs are financially tied to to the owners of recovery facilities.
The so-called pee farms aren’t the only scam that recovery facilities in South Florida have been accused of. Though referral kickbacks — in which a health care provider gives a person or organization money or favors in exchange for providing them with patient referrals — are illegal in Florida, the practice is common and often referred to as “patient brokering,” Steiner said.
Steiner, a registered nurse, has been working in recovery in Delray Beach for 35 years. She’s seen it all, including labs cold-calling her soliciting a partnership in the urinalysis scam.
According to Steiner, outpatient programs and rehabs often hire people to get recovering addicts back into treatment, pointing them toward specific programs — and even giving them cash in hopes that they will buy drugs and need to go back into rehab.
“You’re getting a vulnerable population, they’re 60 or 90 days clean, they’re struggling every day,” Steiner said. If someone in early sobriety is offered money to go buy drugs, she added, it’s hard to turn down.
Even without these bad actors, programs that insist on abstinence-only models are fighting an uphill battle against the realities of opiate addiction.
Research has overwhelmingly shown that the most effective way to keep people from dying is to use medications such as methadone or buprenorphine, long-acting opiates available by prescription from doctors and clinics with specialized certifications and regulations.
“If you look at the data, it’s hard to argue against medication,” said Jeffrey Samet, the medical director of the addictions division of the Boston Public Health Commission, told BuzzFeed News. “The fact that it’s an opioid — who cares?”
Heroin and painkillers like oxycodone are short-acting, which means that within hours of getting a fix, addicts are back on the street hustling for more. Because opiate users quickly develop a tolerance to the drugs, after a while they’re using not to get high but rather to keep the physical and mental pain of withdrawal at bay.
In contrast, opiates such as buprenorphine, sometimes mixed with a drug called naltrexone that curbs the high users feel when taking opiates, can stave off withdrawal and stabilize addicts’ lives. And because they are maintaining their tolerance, if they do relapse, they’re much less likely to die: Studies have shown buprenorphine and methadone cut the overdose risk in half.
“You try to talk to treatment providers in Delray Beach about medication-assisted treatment and they’ll look at you like you’re the spawn of Satan.”
“We preferentially offer people these other treatments [like rehab] that are socially acceptable to people, until they are so debilitated they can’t function,” Melinda Campopiano, a medical officer at the federal Substance Abuse and Mental Health Administration, told BuzzFeed News. “It’s like waiting until they have a stroke and saying, 'Oh, you really are sick, now you can have this medicine.'”
But opiate treatment is a tough sell in Delray Beach, where the recovery community is built largely on 12-step programs that preach abstinence.
“You try to talk to treatment providers in Delray Beach about medication-assisted treatment and they’ll look at you like you’re the spawn of Satan,” Cassidy, who said his treatment center is the only one in Delray Beach that offers methadone, suboxone, and other addiction medications, told BuzzFeed News.
Regardless of what type of treatment they feel comfortable with, struggling addicts looking to get clean should ask a lot of questions about the program they’re entering, Kathleen Carroll, a professor of psychiatry at Yale University School of Medicine who studies addiction treatment, told BuzzFeed News.
“Ask what evidence-based therapies they provide, ask what medicines they provide, ask about their outcomes. If you don’t hear good answers, don’t go there,” Carroll told BuzzFeed News. “Don’t believe what you see on TV — that’s not real. It takes time and work. There’s no magic cure.”

The Delray Beach community, and Florida at large, is increasingly working to combat the fraud and negligence that has grown in the city’s dark corners.
The Delray Beach Drug Task Force, a nonprofit consortium of law enforcement agencies, treatment providers, and other people involved in the addiction industry, runs education and health initiatives and meets regularly to discuss better solutions.
“We’re working with a vulnerable population, and vulnerable populations need consumer protection from those who may not be providing ethical services,” Suzanne Spencer, the executive director of the task force, told BuzzFeed News.
One way to stop the fraud would be to stop the money, according to Steiner, who runs The Sanctuary in Delray Beach.
“I’m praying the insurance companies are cracking down,” Steiner told BuzzFeed News. “I live in Delray, I love Delray. We have a very successful recovery community — these few people and places, it’s sad for the rest of us who do the right thing.”
So far there has been one lawsuit against a Florida lab for urine testing scams: In 2013, Blue Cross Blue Shield sued a lab for fraudulent billing. (The lawsuit is ongoing.)
Recent legislation might also help curb corruption. This summer Florida Governor Rick Scott signed a bill mandating that the recovery residence community come up with a voluntary certification program for halfway houses. Rehabs legally will only be allowed to refer graduates to certified residences.
This summer also saw the state legislature expanding access to the overdose prevention drug naloxone, making it easier for doctors to write just-in-case prescriptions for people who are most likely to encounter someone in the middle of an overdose.
And there’s been a major push toward medication-assisted treatment nationwide. The Substance Abuse and Mental Health Administration, for instance, is pushing states to require rehabs to provide medications like naltrexone, buprenorphine, and methadone. Even the old-guard rehab centers like Betty Ford and Hazelden have started providing medication-assisted treatment.
And the Delray Beach community, long a stronghold for abstinence-only programs, is also beginning to consider other options.
“These are ideas we never thought we’d have to consider,” Spencer, the task force director, told BuzzFeed News. “It’s so much more than a treatment protocol. It’s about a mentality and a culture.”
Still, these changes are slow-moving, and come too late for many people who went to Florida looking for help.

Nicole’s family’s lawsuit against Halfway There is ongoing, even though the place has shut down.
“The corporate entity is still active and even if it wasn’t — there are laws about how long the corporation is responsible after it closes,” the family lawyer, Susan Ramsey, told BuzzFeed News by email. Halfway There could be responsible for several more years, she added. “There is a question about who might pay a judgment but we will cross that bridge when we get there.”
The suit is asking for $15,000 in damages, though Myra Cronin told BuzzFeed News that it’s not about the money. Her family wants national attention on the corrupt industry that they believe cost Nicole her life.
“I don’t think people should be able to profit at the expense of young people’s lives,” Myra said. “Nicole doesn’t have a voice anymore, so I have to talk for her.”
CORRECTION
An earlier version of this article incorrectly stated that American Addiction Centers owns a lab that is being sued for fraudulent billing.
CORRECTION
Studies have shown buprenorphine and methadone, not morphine, cut the overdose risk in half.
