
On Thursday, President Obama signed an executive order laying out the national HIV/AIDS strategy for the next five years. The plan is fairly similar to the old strategy, with one big exception: It focuses on a pill that can prevent people from becoming infected with HIV.
The once-a-day pill, Truvada — used to prevent HIV in what's known as pre-exposure prophylaxis (PrEP) — was approved by the FDA in 2012. When taken every day, studies show, Truvada reduces the likelihood of contracting HIV by at least 92%.
Since its debut, the drug has been heralded as the key to finally turning the tide on new HIV infections. Federal health officials have strongly recommended its use for people at risk of contracting the virus.
But Truvada is also riddled with stigma. Some associate the drug with a freewheeling promiscuity that forgets the devastating impact AIDS once wrought. As Out put it, Truvada is not only a little blue pill, it's "a generation's worth of fear and PTSD, coated in the promise of a new age of sexual freedom."
That stigma has fueled further misunderstandings about how exactly the drug works, whether it's safe, and who should take it. So while researchers and clinicians initially braced themselves for a swarm of interest, uptake of the drug has been slower than predicted.
The drug's maker, Gilead, has so far tallied that only 8,512 people have been prescribed the drug for preventative use since it was approved. The real number is higher than that, as Gilead's data comes from just 39% of U.S. pharmacies. Still, it's far lower than the number of people who could benefit from the pill: The rate of new HIV infections in the U.S. still hovers around 50,000 per year.
Which is why the Obama administration's new push on PrEP matters.
"It acknowledges where progress has been made, but also where we need more," Mitchell Warren, executive director of AVAC, a global HIV-prevention advocacy group, told BuzzFeed News. "If the ambition of the new strategy is to reduce new infections, that's not going to happen with business as usual."
That also requires clearing the misconceptions still hanging over the pill, which while not perfect, has the potential to change the face of an epidemic. Here are six things science has taught us about PrEP.
1. PrEP isn’t a magic bullet, but missing a single dose doesn’t mean you’re screwed, either.

The big word here is "adherence." Although PrEP is roughly 92% successful at warding off new HIV infections when taken properly, it's hard to tell how many people will manage to stick to the once-a-day regimen recommended by the CDC.
The results of several year-long studies on adherence were revealed last week at the International AIDS Society meeting in Vancouver.
"We wanted to look at outside of a clinical trial and ask, when PrEP is provided in normal life settings, what is adherence like? Are people able to take the drug on a regular basis?" Albert Liu, research director of the HIV prevention program at the San Francisco Department of Public Health and the lead investigator on one of the studies, told BuzzFeed News.
Liu's study, which will be published in the next few months, oversaw 557 patients — either men who have sex with men (MSM), or transgender women — visiting clinics in San Francisco, Miami, and D.C. The study provided one year of Truvada, along with STI testing, counseling, and clinical monitoring. In exchange, some of the volunteers underwent routine blood draws to see how well they were sticking to the drug.
After a year on Truvada, 63% of volunteers showed levels of the drug in their blood that consistently corresponded to taking it four or more times per week, the study found.
Although four times a week is lower than the CDC's daily recommendation, studies suggest that it is likely enough to provide high levels of protection for MSM. Only two patients in the study contracted HIV, and both had blood levels that indicated they weren't taking the drug at all.
"We do think that taking daily dosing provides the most forgiveness, and also fosters establishing a daily routine for taking the pills, which many people appreciate," Liu said.
In other words, while a daily dose is still the best guarantee against contracting HIV, missing a single pill is most likely not going to hurt you.
Liu's results also indicate that most MSM and trans women can effectively incorporate Truvada into their health routines.
For some, however, a daily pill just isn't the right fit. "There are some people who aren't going to adhere ever, and Truvada is not going to work for them," Warren said. "And that's why we still need other options."
Other forms of PrEP are in development that might help with the adherence issue. Many of these match existing contraception techniques: a ring, injectables, and implantables. In the meantime, there are always condoms.
2. There’s no evidence that PrEP makes people more likely to engage in risky behavior.

Much of the initial pushback to Truvada came from a few prominent voices putting forth the idea that the pill would lead to more sex and fewer condoms.
Most famously, Michael Weinstein, president of the Los Angeles-based AIDS Healthcare Foundation, the largest HIV/AIDS medical care provider in the U.S., called Truvada a "party drug" and implied it would lead to more barebacking, or having anal sex without condoms.
But gay men putting their PrEP status on Grindr doesn't translate to greater amounts of risky sex. The reality is that many people are already taking risks, Truvada or no Truvada.
"You feel the moralism creeping in," Warren said. "What if everyone takes PrEP and stops using condoms? Well, if everybody used condoms I would share that concern, but we would not have a raging epidemic if everyone used condoms."
Liu and Warren both stressed that no study of PrEP to date has shown any correlation with riskier sex. Liu's recent study, which also asked volunteers to report their number of sexual partners, actually showed a decrease in partners over the three-month reporting period, dropping from 11 to 9. The amount of condomless sex stayed relatively stable. Previous studies also did not find increases in partner number post-Truvada.
The decrease in sexual partners in Liu's own study, he said, may have to do with the fact that being on a once-a-day medication brings many people into the health care system who otherwise wouldn't have been, perhaps making people more aware of decisions that could impact their health.
"Getting someone into the clinic every three months, getting them to know their HIV status? That's huge!" Warren said. "We should be celebrating that."
3. Despite the rumors, using PrEP won’t lead to a mutated, drug-resistant form of HIV.

Like many of the misconceptions around PrEP, this one is wrapped up in stigma, Warren said. But the science is simple: You can't have drug resistance without being infected with HIV.
Since PrEP is only intended to be used by people who test negative for HIV, there would be no virus in their blood to develop resistance to Truvada in the first place. "The takeaway is: no infection, no resistance," Warren said.
Resistance has happened, very rarely, in PrEP trials when someone is "acutely" infected with HIV — meaning that they have only been infected for days or weeks, not long enough to produce a positive test result. Someone with this hidden HIV infection could be accidentally prescribed PrEP and develop resistance to the drug, but the chances of that are low, and it would be quickly caught by the patient's doctor.
In Liu's study, three volunteers were acutely infected. One of them developed resistance to one of the compounds in Truvada, but it was detected quickly and he was immediately switched to an HIV treatment regimen. Now his HIV infection is fully suppressed.
"It really highlights the importance of trying to rule out acute HIV infection when people are starting PrEP," Liu said.
4. Lots of different people use PrEP, for lots of different reasons.
Researchers across the world are working on roughly 35 "demonstration projects" like Liu's, testing how well Truvada will be used in the real world among specific slices of populations at high risk of contracting HIV.
Those trying out the drug include heterosexual men and women in Botswana, young black men in California's Bay Area, people who inject drugs in Thailand, female and transgender sex workers in India, and committed couples in which one individual is HIV positive and the other is negative in Nigeria.
For each of these situations, the pill on its own will not lower HIV infection rates. Each setting will require researchers to use specific outreach strategies to find and talk to people at risk, and see what works best for them.
In the U.S., for example, young black and Latino men are less likely to take Truvada than other groups are, despite the fact that both populations are disproportionately affected by HIV.
According to Liu, whose study also showed lower adherence rates among black men, it may boil down to "stigma, discrimination, and social factors."
5. PrEP does not protect against other sexually transmitted diseases.

Unlike condoms, PrEP only defends against one bug: HIV. People who are having unprotected sex and using Truvada should be cautious of their risk of contracting other STIs.
STI rates among Liu's study population were high — hovering around 25% — before and during his year-long study.
Although his study didn't show increased rates of STIs after Truvada use, clinicians need to be diligent to test for them. The good thing, though, is that individuals on a PrEP regimen are integrated into the health care system and so will receive more monitoring than they otherwise might.
For the highest level of protection, especially when a partner's STI status is unknown, it's best to combine Truvada with condoms. "Every method is imperfect," Warren said. "No one method should replace another. It's additive."
6. PrEP does come with some side effects — but they are usually manageable.
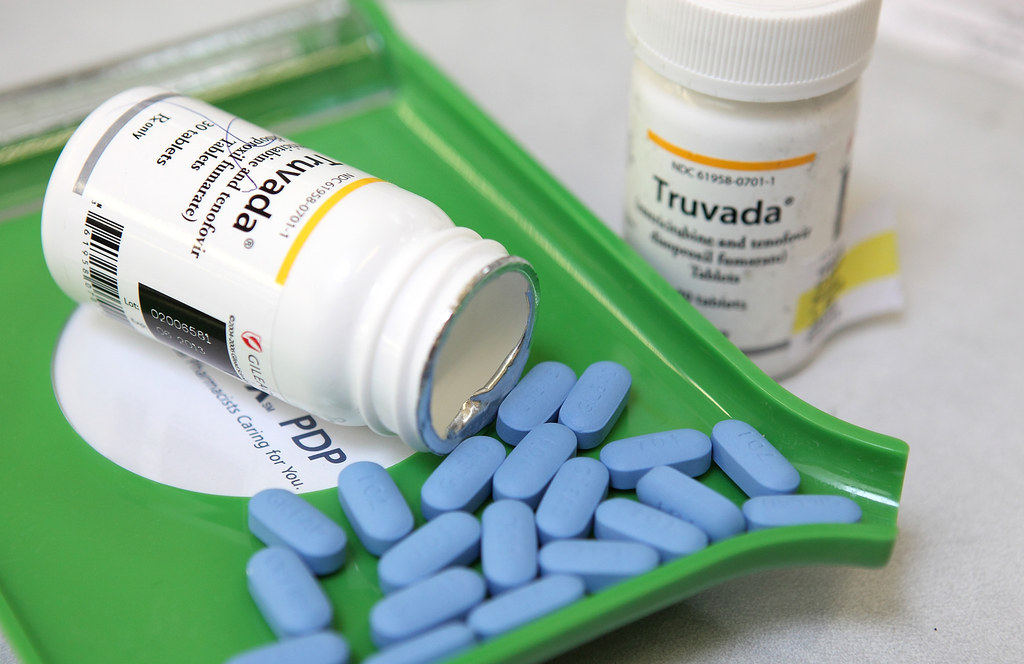
Like any drug, Truvada comes with some side effects. The most common (experienced by 5% or more people to take it) are nausea, abdominal cramping, vomiting, dizziness, fatigue, and diarrhea, but those most often resolve in the first month of taking the drug.
Anecdotally, many people worry about a potential loss of bone density and kidney function, which have cropped up in some HIV-positive people who take Truvada in combination with other drugs. But so far these side effects haven't been seen in healthy people taking the pill to prevent HIV infection.
"None of us should be wildly promoting PrEP without talking about side effects," Warren said, "but nothing has come up yet that anyone can say is a grave concern."
But unlike HIV treatment, PrEP should not be thought of as a lifelong regimen, he added. It's meant for otherwise healthy people during riskier periods of their lives. "No one is suggesting people should go on PrEP for life."
Liu's study showed lower adherence rates for Truvada among black men. Other studies have shown that Latino men are less likely to take Truvada, but don't have lower adherence rates, as an earlier version of this post misstated.
